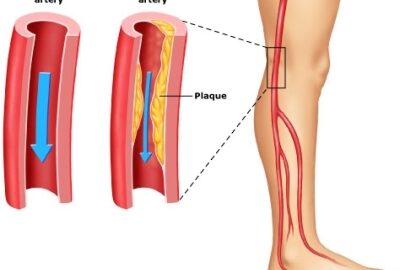
Peripheral artery disease (PAD), also known as peripheral vascular disease (PVD), is a very common condition affecting 20 percent of Americans age 65 and older. Peripheral Artery Disease (PAD) develops most commonly as a result of atherosclerosis, or hardening of the arteries, which occurs when cholesterol and scar tissue build up, forming a substance called plaque inside the arteries. This is a very serious condition, therefore needing attention. The clogged arteries cause decreased blood flow to the legs. This can result in pain when walking, and eventually gangrene and amputation.
Because atherosclerosis is a systemic disease (that is, affects the body as a whole), individuals with Peripheral Artery Disease (PAD) are likely to have blocked arteries in other areas of the body. Thus, those with PAD are at increased risk for heart disease, aortic aneurysms and stroke. Peripheral Artery Disease is also a marker for diabetes, hypertension and other conditions. Blood clots may also be a cause of Peripheral Artery Disease.
Peripheral Artery Disease Symptoms
Intermittent Claudication is the most common symptom of Peripheral Artery Disease PAD. Intermittent claudication is painful cramping in the leg or hip that occurs when walking or exercising and typically disappears when the person stops the activity.
- Numbness, tingling and weakness in the lower legs and feet
- Burning or aching pain in feet or toes when resting
- Sore on leg or foot that won’t heal
- Cold legs or feet
- Color change in skin of legs or feet
- Loss of hair on legs
- Have pain in the legs or feet that awakens you at night
- Many people simply live with their pain, assuming it is a normal part of aging, rather than reporting it to their doctor.
Prevalence
PAD is a disease of the arteries that affects 10 million Americans.
Peripheral Artery Disease (PAD) can happen to anyone, regardless of age, but is most commonly seen in men and women over age 50.
What are the Risk Factors
Those who are at highest risk for PAD are
- Over age 50
- Smokers
- Diabetic
- Overweight
- Inactive (and do not exercise)
- Have high blood pressure or high cholesterol or high lipid blood test
- Have a family history of vascular disease, such as PAD, aneurysm, heart attack or stroke
How can you Diagnose PAD
The most common test for PAD is the ankle-brachial index (ABI). An ABI is an exam that uses ultrasound and a blood pressure a cuff to measure the ratio of blood pressure in the feet and arms. Your doctor will use the ABI results as well as symptoms and risk factors for PAD to decide if further tests are needed. Sometimes a doctor may order an imaging technique called magnetic resonance angiography (MRA) or with computed tomography (CT) angiography.
Ankle-Brachial Index (ABI)
Peripheral Artery Disease (PAD) is a major public health issue, and the Society of Interventional Radiology recommends greater screening efforts through the use of the ankle-brachial index (ABI) test.
The ABI is a simple, painless test that compares the blood pressure reading in the arm and ankle. It is a direct measure of fatty plaque buildup in leg arteries and an indirect gauge of plaque accumulations throughout the entire cardiovascular system.
Blood pressure cuffs and a special ultrasound stethoscope called a doppler compare the pressure in your arms and legs.
An individual with an ABI of 0.3 (high risk) has a two- to three-fold increased risk of five-year cardiovascular death compared to a patient with an ABI of 0.95 (normal or low risk).
Ultrasound doppler uses sound waves to produce images that highlight blood flow in the leg arteries and veins. This test detects and evaluates any blockages caused by plaque buildup.
You can learn more about testing here: Leg Circulation Tests.
Peripheral Artery Disease Treatments
Lifestyle Changes
Lifestyle changes can help with treating Peripheral Artery Disease (PAD). You can alleviate symptoms and prevent further progression of the disease with and exercise program or by quitting smoking.
Medication
Medications that lower cholesterol or control high blood pressure may be prescribed. Medication available, has sometimes shown to significantly increase pain-free walking distance and total walking distance in individuals with intermittent claudication. Other medications that prevent blood clots or the buildup of plaque in the arteries are available as well.
Angioplasty and Stenting
Interventional radiologists pioneered angioplasty and stenting, which was first performed to treat peripheral artery disease. Using imaging for guidance, the interventional radiologist threads a catheter through the femoral artery in the groin, to the blocked artery in the legs. The interventional radiologist then inflates a balloon to open the blood vessel where it is narrowed or blocked. If plaque blocks the vessel, the doctor will use a stent. A stent is a tiny metal mesh cylinder. This is a minimally invasive treatment that does not require surgery, just a nick in the skin the size of a pencil tip.
Balloon angioplasty and stenting have generally replaced invasive surgery as the first-line treatment for PAD. Early randomized trials have shown interventional therapy to be as effective as surgery for many arterial occlusions. Clinical experience in centers throughout the world has shown that stenting and angioplasty are preferred as a first-line treatment.
Atherectomy
An atherectomy is a procedure that utilizes a catheter with a sharp blade on the end to remove plaque from a blood vessel. The catheter is inserted into the artery through a small puncture in the artery. At the site of blockage the tool is able to “shave” or “cut” the plaque from the inside of the artery and remove it from the patient.
Stent-grafts
A stent-graft is a device constructed from a stent and a vascular conduit that is inserted using catheter techniques and image guidance. The stent serves to anchor the graft in the blood vessel lumen, and in most cases provides structural support for the graft material. The graft material provides a conduit for blood flow.
Surgery
Blockages from arteries sometimes require invasive open surgery. This procedure bypasses the clogged area. Invasive open vascular surgeries are usually performed in a hospital. These types of procedures are much more expensive and usually require a longer stay and recovery time.
Are You at Risk for Peripheral Artery Disease (PAD)?
Call 727-475-4039 for a consultation.
For more information on Peripheral Artery Disease, you can visit the American Heart Association.